A lot of patients contact us wanting to know about alternatives to CPAP for the treatment of Obstructive Sleep Apnoea (OSA). Although CPAP is a critical treatment option for many who suffer from OSA, new technology and treatment options are offering great results for many patients
What is OSA?
Obstructive sleep apnoea (OSA) is a common medical condition affecting around 25% of the adult population. It is one of many sleep breathing disorders, and OSA involves the collapse of the soft tissue of the upper airway, resulting in a partial or complete blockage of breathing.
Symptoms differ from person to person, but usually involve some degree to tiredness or sleepiness during the day, and can be associated with snoring. However, many cases of OSA go undiagnosed for years.
The biggest concern usually for patients with OSA is how it interferes with day-to-day life. They can find it easy to doze off during the day, or difficult to concentrate. OSA has also been associated with increased blood pressure and increased risk of cardiovascular events.
How is OSA diagnosed?
Diagnosis is confirmed by a sleep study, completed at home or at a sleep centre. This study is analysed by a Sleep Physician, who assesses the data. Typically, someone will have a partial or complete obstruction of the airway 0-5 times per hour. This value is called the Apnoea-Hypopnoea Index (AHI) and anything 5+ is OSA. The severity of OSA is dependent on the AHI, with 5-15 being mild, 15-30 moderate, and >30 severe.
How is it managed?
Management is divided into four main categories: lifestyle/behavioural changes, continuous positive airway pressure (CPAP), oral appliance, or surgery. The best option for each person is an individual thing and discussion with your treating Sleep Physician or ENT is incredibly important. A combination of things is usually required to manage the OSA.
It is also important to note that we have yet to find an
absolute cure for OSA, and treatment is more about the management of the
condition.
How does a dentist come into this?
Although a CPAP is widely regarded as giving the best outcome for patients with OSA, the device, which fits over the nose and sometimes the mouth too, can be bulky and cumbersome. Mild and moderate cases, and even sometimes severe cases, can be recommended to have an oral appliance made.
An oral appliance (OA) has many names, including a mandibular advancement device (MAD) or mandibular advancement splint (MAS). There are over-the -counter options available, but for most people they tend to be uncomfortable.
This is where a dentist comes in. We make custom fitted devices to help with management of the OSA, as well as help with the adjustments and reviews to make sure the device works best for you.
How does a MAS work?
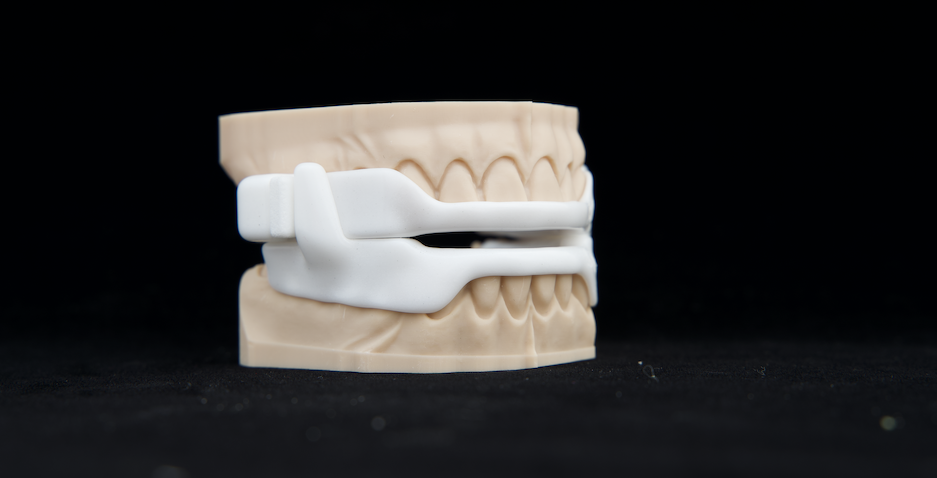
The device fits over your top and bottom teeth and holds or pushes the lower jaw forward. This forward position means that there is more space behind your throat and allows air to pass through.
A patient then wears the device every night when going to sleep. Easy as that.
How is a MAS made?
A mould of your teeth is taken; either digitally or physically. Usually this involves taking an impression of your teeth like you would have for custom mouthguards. This mould is sent to our lab for the device to be made, using measurements that we have taken during the appointments.
The material used these days is mostly 3D-printed nylon, but acrylic is sometimes used to.
When the device comes back, the dentist will fit it and make
sure it is comfortable and you are pretty much good to go! The device is able
to be titrated – meaning that we adjust how far forward we move the jaw to get
the best result for your OSA. We will get you back in at least 4-6 weeks after
the device is fitted, and on a yearly basis as well. However, we will get you
in if there are any issues at any point with the device.
How do I get a MAS?
Firstly, we need to make sure we have a diagnosis and treatment plan from your treating physician. This is usually a Sleep Physician or ENT specialist. We need this to know we are managing the right condition, and also as a baseline for future reviews. We can use the first diagnosis / sleep study to see if we have made improvements in the future.
To get a proper diagnosis either approach a GP or have a home sleep study completed.
Once the report has returned from your sleep study, there will be recommendations for treatment options. An oral appliance is usually recommended for patients to try, but it is not always appropriate. Hence it is important that the Sleep Physician or ENT specialist has recommended it. Do note that a MAS is not always successful for management of OSA, especially as the severity of the condition increases. If you have the above, then the dentist will see you for a consultation and examination. As long as the teeth and oral tissues are stable and healthy enough to proceed with the device then impressions can be taken and the process started.
Opening Hours:
Mon: 8am – 5pm
Tue: 8am – 7pm
Wed: 8am – 6pm
Thu: 8am – 5pm
Fri: 8am – 5pm
Sat: 8am – 1pm
Sun: Closed






